We Can Do Better
I’ve waited a long time to tell this story. In fact, my heart is beating out of my chest as I type. It’s not even really a bad story -- trust me, working with postpartum women I have heard some horrible birth stories. But it’s a story that is very personal to me. I take it personally because it’s my body, it was my own naive understanding of how maternal care works in this country, so I feel tricked. It’s also personal because now my absolute mission, in life and at Mind the Mat, is to advocate and support the highest level of prenatal and postpartum care for women in this country. We deserve it. I knew it was time to tell my story because when I read articles with staggering statistics like the U.S. Has the Worst Rate of Maternal Deaths in the Developed World, I would feel a burning anger inside me. Or, when I recently attended the largest physical therapy conference in the world this month, right here in Washington D.C., I sat at attention in women’s health programming that reported important evidence-based treatment methodology. It's methodology that, if implemented across the board, which can be done easily, can immediately help women before and after birth. But, and this is frustrating, these evidence-based practices are not actually common in this country.So when I got angry or choked up throughout that programming, I realized I hadn’t fully processed what had happened, I hadn’t worked through it. I knew it was time to tell my story. And now that I have Mind the Mat as a platform, I want to positively channel that energy into helpful programs for the good of all women.I had a relatively easy pregnancy. I admit we were blessed. I was 31 and conceived pretty easily, within about five months. I was active and happy being pregnant. I even annoyingly said to people, “I don’t know why anyone complains about being pregnant, it’s so great.”I had charted my fertility using the book Taking Charge of Your Fertility so I truly felt I knew the exact date of conception. I had chosen a midwife-based practice to ensure I had a better chance of having a natural delivery…I felt like I had checked all the right boxes in planning (and I am not a planner!).My OB practice did not allow moms to go more than a week past their due date, so when my due date came and went, I was getting frustrated, impatient, and nervous. Because of this “rule,” I had to schedule a visit with an OB in this practice I'd not yet seen as he was the only doctor with an appointment available that day. I expressed my concerns about being induced and told him I could pinpoint my conception date so maybe my due date was off. He looked at me like I was crazy and seemed irritated that I would even suggest such a concept. “Our due date calculations are correct,” he said, tersely, as he annoyingly parted my knees to give me an exam.I felt like I was wasting his time, that he was the doctor and he knew best.Being in the medical/health care community myself, I trusted that practice to do right by me and my baby. I went in for my scheduled induction and, from the start, things just weren’t right. I’d always heard of my friends checking in to the hospital at night then delivering their babies the very next day. I wasn’t naive enough to think that would necessarily be me, a quick few hours and hello, baby. But I remember hearing a nurse comment that the scheduling of the induction was wonky and that she’d never seen a doctor plan it out that way. Odd, and not a great feeling. Still, I knew I was in good hands.I labored through he night on Pitocin (the drug that makes the uterus contract, it ain’t pretty) without any pain meds…I still wanted to try to have a natural delivery. The nurses who cared for me that night were unreal — so amazing, so pro-women. I wish I could remember who they were. I do remember one bad-ass nurse locking eyes with me as I was laboring. She said, “I know what you are trying to do. You are strong. You are. But please know you won’t be a failure if you decide to get an epidural.”That morning after I finally agreed to some kind of narcotic to help me sleep, the doctor walked in to explain that my baby’s heart rate was not ebbing and flowing as it should. I asked if I could change position, if that would help since I had been laboring on my back all night...but they said no. I didn’t want my baby’s safety compromised, even if there were only a slight chance. So they wheeled me in for a c-section. I was not going to object.The gist of this birth story is this: I had a baby, he was healthy, he didn’t feed well (don’t get me started on breastfeeding…the guilt, the pressure, the confusion of whether to use formula or not with a jaundice baby, the rift between pediatricians and lactation specialists; just know it doesn’t always come easily to moms and please give people a break). But we worked through it and Luke was okay.
I knew it was time to tell my story because when I read articles with staggering statistics like the U.S. Has the Worst Rate of Maternal Deaths in the Developed World, I would feel a burning anger inside me. Or, when I recently attended the largest physical therapy conference in the world this month, right here in Washington D.C., I sat at attention in women’s health programming that reported important evidence-based treatment methodology. It's methodology that, if implemented across the board, which can be done easily, can immediately help women before and after birth. But, and this is frustrating, these evidence-based practices are not actually common in this country.So when I got angry or choked up throughout that programming, I realized I hadn’t fully processed what had happened, I hadn’t worked through it. I knew it was time to tell my story. And now that I have Mind the Mat as a platform, I want to positively channel that energy into helpful programs for the good of all women.I had a relatively easy pregnancy. I admit we were blessed. I was 31 and conceived pretty easily, within about five months. I was active and happy being pregnant. I even annoyingly said to people, “I don’t know why anyone complains about being pregnant, it’s so great.”I had charted my fertility using the book Taking Charge of Your Fertility so I truly felt I knew the exact date of conception. I had chosen a midwife-based practice to ensure I had a better chance of having a natural delivery…I felt like I had checked all the right boxes in planning (and I am not a planner!).My OB practice did not allow moms to go more than a week past their due date, so when my due date came and went, I was getting frustrated, impatient, and nervous. Because of this “rule,” I had to schedule a visit with an OB in this practice I'd not yet seen as he was the only doctor with an appointment available that day. I expressed my concerns about being induced and told him I could pinpoint my conception date so maybe my due date was off. He looked at me like I was crazy and seemed irritated that I would even suggest such a concept. “Our due date calculations are correct,” he said, tersely, as he annoyingly parted my knees to give me an exam.I felt like I was wasting his time, that he was the doctor and he knew best.Being in the medical/health care community myself, I trusted that practice to do right by me and my baby. I went in for my scheduled induction and, from the start, things just weren’t right. I’d always heard of my friends checking in to the hospital at night then delivering their babies the very next day. I wasn’t naive enough to think that would necessarily be me, a quick few hours and hello, baby. But I remember hearing a nurse comment that the scheduling of the induction was wonky and that she’d never seen a doctor plan it out that way. Odd, and not a great feeling. Still, I knew I was in good hands.I labored through he night on Pitocin (the drug that makes the uterus contract, it ain’t pretty) without any pain meds…I still wanted to try to have a natural delivery. The nurses who cared for me that night were unreal — so amazing, so pro-women. I wish I could remember who they were. I do remember one bad-ass nurse locking eyes with me as I was laboring. She said, “I know what you are trying to do. You are strong. You are. But please know you won’t be a failure if you decide to get an epidural.”That morning after I finally agreed to some kind of narcotic to help me sleep, the doctor walked in to explain that my baby’s heart rate was not ebbing and flowing as it should. I asked if I could change position, if that would help since I had been laboring on my back all night...but they said no. I didn’t want my baby’s safety compromised, even if there were only a slight chance. So they wheeled me in for a c-section. I was not going to object.The gist of this birth story is this: I had a baby, he was healthy, he didn’t feed well (don’t get me started on breastfeeding…the guilt, the pressure, the confusion of whether to use formula or not with a jaundice baby, the rift between pediatricians and lactation specialists; just know it doesn’t always come easily to moms and please give people a break). But we worked through it and Luke was okay.
I, however, was not great.
I was in severe pain. My c-section incision was painful and affecting my mobility and my ability to care for my baby and myself. I returned for my six-week postpartum checkup and explained my limitations to the doctor. He listened, then immediately after I told him I couldn’t move at the end of the day he asked, “So what are you doing for birth control?” I responded with, “C-section. I am using a painful and concerning slow-healing c-section incision as my birth control.”I am also absolutely convinced that I had severe postpartum depression. I only realized this after I had my second baby (also via c-section) and felt completely different. Postpartum depression doesn’t necessarily look like we’d expect. You don’t have to feel sad, although that could be a symptom. For me, I could not get myself together and I had crippling anxiety. I couldn't get out the door. I was a wreck all the time. I thought it was just part of having a baby.But did you know there is a reliable and valid tool that doctors can use that helps assess for postpartum depression? I did not receive that assessment, nor did anyone involved in my aftercare ask me a single question about my mental state or ability to function as a human being, much less care for a newborn baby.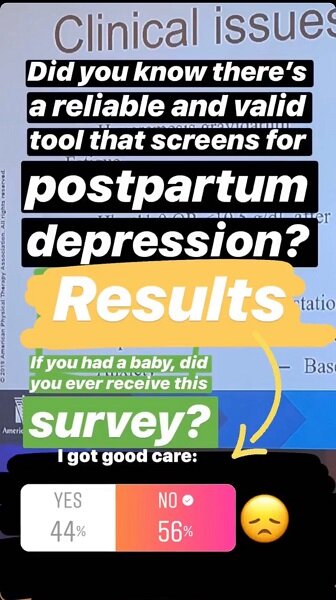 In conclusion, I would like to outline my postpartum care after having major surgery: There, did you get that? I’ll outline it again for you in case you think there is something wrong with your screen: Now I have to mention the disclaimer here. There seems to be some sentiment in our society and among other women to toughen up, suck it up, and be superhuman. Be a mom. Women have done it for thousands of years and you have a healthy baby, so don’t talk about the hard things, everyone goes through them.No. Just, no.
In conclusion, I would like to outline my postpartum care after having major surgery: There, did you get that? I’ll outline it again for you in case you think there is something wrong with your screen: Now I have to mention the disclaimer here. There seems to be some sentiment in our society and among other women to toughen up, suck it up, and be superhuman. Be a mom. Women have done it for thousands of years and you have a healthy baby, so don’t talk about the hard things, everyone goes through them.No. Just, no.
Not anymore. Those days need to be over. We need to talk about this and admit that although we are Wonder Women, our bodies and minds can suffer in response to the beauty of giving life, and we don’t have to “accept it.” In my next post, I will outline some evidence-based treatment options and plans that can overhaul our postpartum care for women and hopefully elevate us past third world country status when it comes to caring for our mothers.
And if you think this does not relate to you (you are a man, you are not a mom, etc.) we were all born. We all have or had a mother…so this should affect us ALL.